
Share this post!
A Course in Nutrition: Learning Your A, B, C’s
Welcome back to part 10 of our multi-part series on vitamins. This one is all about vitamin D: the sunshine prohormone!
In the last blog of the series, we talked about vitamin C.
We highlighted:
- Forms of vitamin C
- Its roles in the body as an antioxidant and cofactor for metabolic reactions
- Optimal levels and deficiency
- Recommended intake
- Food sources and a green-pea hummus dip recipe
Next, we move on to vitamin D, which is not technically a vitamin because the human body can synthesize it in adequate quantities.
Vitamin D is fascinating. We’ll discuss the forms of vitamin D and how it’s metabolized, its roles in the human body, dietary sources, optimal levels, and a recipe. Let’s get into it!
Vitamin D: Forms, Activation, and Metabolism
Vitamin D is a fat-soluble nutrient that can be obtained from the diet in two forms:
- D2, or ergocalciferol, is derived from plants, the best source being mushrooms
- D3, or cholecalciferol, is found in animal products such as fatty fish (sardines, tuna, mackerel, etc.), eggs, liver, and fish liver oils
Vitamin D3 is also the form we synthesize upon skin during exposure to sunlight, specifically UVB radiation. 7-dehydrocholesterol, a derivative of cholesterol, is the precursor to vitamin D3. Since it is possible to synthesize adequate quantities of vitamin D with sunlight, vitamin D is not a true vitamin in the sense that it isn’t necessary to obtain through dietary means alone.
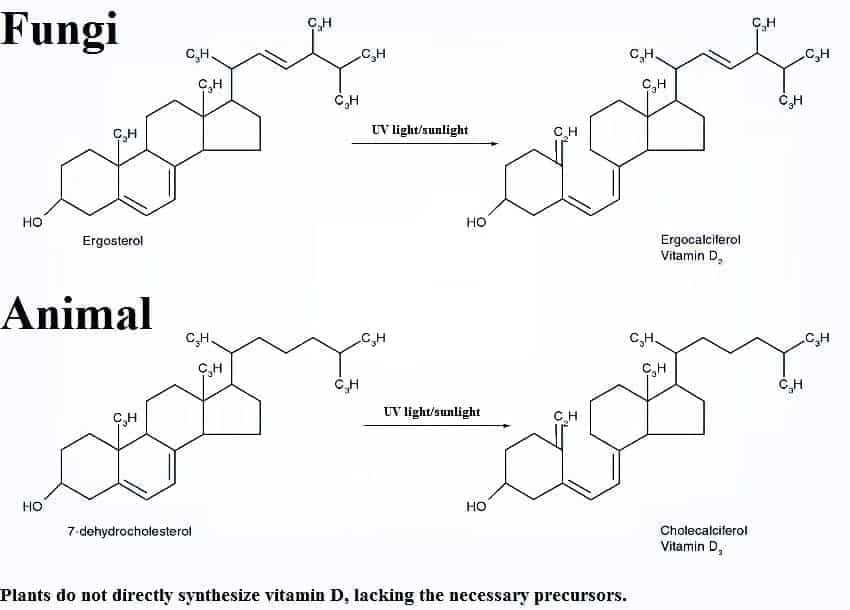
Vitamin D2 and D3, whether from diet or sun exposure, is a prohormone, which is a physiologically inactive precursor of a hormone.
Comversion for Activation
The prohormone vitamin D is converted to calcidiol (25-hydroxy vitamin D) via a hydroxylation reaction (addition of an –OH group) that takes place in the liver. Calcidiol is the storage form of vitamin D. Routine blood tests check for the concentration of this metabolite of vitamin D when assessing nutritional status, as this form lasts in the body for several weeks.
In the kidneys, another hydroxylation reaction converts calcidiol into calcitriol (1,25-dihydroxy vitamin D), the metabolically active form of vitamin D. Once activated, this form of vitamin D lasts only hours in the body before being broken down.
The kidneys are the main regulators of circulating vitamin D levels, as they control how much is activated and broken down. The kidneys prevent circulating vitamin D levels from going too high by secreting an enzyme that inactivates calcitriol by converting it to calcitroic acid, a water-soluble derivative for excretion.
Interestingly, the kidneys aren’t the only cells that can activate vitamin D. Bone and immune cells have the ability to activate vitamin D, which bypasses homeostatic regulation by the kidneys in order to produce higher vitamin D levels in bones or at the site of the infection, in order to achieve some of vitamin D’s effects in the body.
What does vitamin D do?
Remember that vitamin D is a hormone, which is a product of living cells that circulates in bodily fluids to stimulate certain cells and tissues into specific actions. Scientists have discovered receptors for vitamin D in many cells and tissues throughout the body, identifying more than 50 genes this hormone can influence.
Here are a few of the most well-known systems that utilize vitamin D.
Calcium Metabolism and Bone Mineralization
Vitamin D stimulates the small intestine to absorb dietary calcium, encourages the kidneys to reabsorb calcium, and facilitates the removal of calcium from bones, if necessary, to maintain tightly regulated serum calcium levels. Together with parathyroid hormone and other factors, vitamin D influences bone remodeling. It stimulates the formation of osteocalcin, a protein that encourages the mineralization of bones, and also encourages the formation of osteoclasts, which are cells that break down bone to reabsorb its minerals in the event of a calcium deficiency.
Immune System Modulation
Vitamin D modulates the immune system – meaning that it activates certain cells and deactivates others during an immune response. The goal of vitamin D’s modulation is optimal immune function with minimal inflammation. Some mechanisms of vitamin D’s role in immune function include:
- The activation of macrophages and monocytes, which are innate immune cells that seek out, neutralize, and digest pathogens, causes these cells to activate vitamin D, which increases the concentration of the hormone in the area of infection. This effect enhances the effects of these immune cells.
- Vitamin D suppresses the action of antigen-presenting cells, which are cells of the innate immune system that process and present foreign molecules or fragments of pathogens (antigens) on the surface of their cells for recognition by other immune cells. By decreasing the activity of these cells, the immune system becomes more tolerant and produces fewer inflammatory substances.
- Vitamin D also regulates the adaptive immune system, which consists of T-cells and B-cells, by shifting the balance of the types of T-cells from the pro-inflammatory Th1 and Th17 type cells to anti-inflammatory regulatory T cells.
- Activated vitamin D inhibits inflammatory cytokines (communication proteins) while promoting anti-inflammatory cytokines, which help the body return to normal after an immune reaction.
Reproductive Health
- Vitamin D has important effects to the reproductive system, including its involvement in sperm production, egg development, implantation, pregnancy, and the health of the offspring, such as the mineralization of fetal bones. Vitamin D may improve female fertility by reducing the circulation of male hormones, as in polycystic ovary syndrome, PCOS.
What happens when vitamin D is low?
Vitamin D deficiency is fairly common in modern times because we tend to spend more time indoors than our ancestors did. General statistics show that one billion people worldwide are deficient in vitamin D, and 50% of the entire global population may have insufficient levels. The elderly, pregnant and breastfeeding women and young children are at the most risk for developing vitamin D deficiency.
Here are some ways vitamin D deficiency can affect our health:
- Low vitamin D status may affect bone mineralization leading to rickets or osteoporosis. Symptoms such as muscle weakness or pain may occur if vitamin D is low.
- Vitamin D deficiency compromises immune function, leading to increased susceptibility of viral or bacterial infection and poorer health outcomes upon infection. Due to vitamin D’s role in promoting immune tolerance and reducing inflammation, it is a factor in the development of autoimmune diseases.
- Inadequate vitamin D may compromise fertility in both men and women.
How can I increase my vitamin D level?
There are 3 main ways to increase vitamin D:
- Sunlight exposure
- Diet
- Supplementation
The best way to increase vitamin D levels is to expose your bare skin to sunlight without sunscreen. A little goes a long way, as 20 minutes of sunlight exposure on about 40% bare skin is adequate. Depending on the season, your position relative to the Equator, the pigment of your skin (darker skin requires more sunlight exposure to produce vitamin D), and your health status or medications, additional sun exposure and/or supplementation may be necessary to achieve adequate vitamin D levels.
READ MORE >>> Making the Most of Vitamin D During the Summer Months
Consuming foods rich in vitamin D is another way to increase vitamin D levels. Fish, such as salmon, sardines, and mackerel, contain up to 500 IU of vitamin D per serving. Egg yolks, beef liver, mushrooms (exposed to UV light), and fortified products all contain vitamin D.
Beyond sun exposure and dietary sources, supplements are another way to increase vitamin D intake. Tablets, gel caps, and gummies are common supplemental forms of vitamin D. Cod liver oil is also a very rich source of vitamin D, with over 1000 IU per tablespoon.
Though vitamin D is found mostly in animal-based foods, vegans and vegetarians can find supplemental forms of D3 that are not sourced from animals.
Optimal Levels
Optimal blood levels of vitamin D, as calcidiol (25-hydroxy vitamin D) vary, according to the National Institute of Health fact sheet. The Endocrine Society states that vitamin D levels above 30 ng/mL are sufficient, less than 20 ng/mL represents a deficiency, and between 20 and 29 ng/mL is insufficient. The Institute of Medicine considers 20 ng/mL levels to be sufficient for most people, with deficiency defined at 12.5 ng/mL. However, optimal health benefits (beyond levels required for bone mineralization) may necessitate higher levels, between 40 and 60 ng/mL.
Next are some general recommendations for how much vitamin D you need.
How much vitamin D should I take daily?
The recommended dietary allowance for vitamin D is 600 IU for children and adults, 400 IU for children under 1 year, and 800 IU for adults over age 70 and pregnant or breastfeeding women.
Supplementation recommendations are variable and should be determined individually based on health status, environment, lab tests, and consultation with a medical professional. A daily intake of 1000-4000 IU via supplementation is adequate for most people to maintain adequate blood concentration. Higher doses taken weekly or monthly are also common.
Being fat-soluble, vitamin D can be stored in adipose tissue, therefore adequate levels may be maintained over time even if sunlight or dietary sources are scarce. This characteristic also makes it possible to overdo supplementation, hence the recommended upper limit of 10,000 IU per day set by the National Institutes of Health. Vitamin D toxicity, though uncommon, can result in increased calcium levels in urine (hypercalciuria) or in blood (hypercalcemia), causing symptoms including dizziness, nausea, bone pain, frequent urination, and kidney problems.
Vitamin D will be optimally absorbed when consumed with a meal containing healthy fats such as avocado, nuts, seeds, grass-fed butter, or coconut oil. Recall that vitamin D production on the skin begins with a cholesterol-derivative – another reason to keep healthy fats on your plate!
Green Salad with Fatty Fish and Olive Oil Vinaigrette
The following recipe is quick, easy, and rich in vitamin D, healthy fats, and other supporting nutrients for bones and immunity, such as vitamin K, calcium, and magnesium. It is my absolute favorite salad to make because it is so convenient and satisfying.
Ingredients:
- Greens – romaine, spinach, kale, chard, parsley – or a combination to your taste and availability
- Can of sardines or mackerel, packed in olive oil, or salmon cooked your favorite way
- Additional morsels, such as pumpkin seeds, capers, feta cheese, avocado, hard-boiled egg, sauerkraut, walnuts – whatever you fancy!
- For vinaigrette: one clove of smashed garlic, 1 tsp mustard, 2 Tbsp apple cider vinegar, 2-4 Tbsp olive oil, 1 Tbsp flax seed oil (optional)
Directions:
Whisk vinaigrette ingredients with a fork in a bowl, or blend with an immersion blender. Drizzle over the remaining salad ingredients. Enjoy as a picnic lunch in the sun, if weather permits!
About the author
Karyn Lane is working towards her holistic nutrition certification in NTI’s Nutrition Therapist Master Program. She finds her chemistry degree a useful tool in her study of holistic nutrition and loves to treat herself as a laboratory for new recipes and cooking techniques. You can follow her on Instagram @feel.alive.nourishment.
About Nutrition Therapy Institute’s Holistic Nutrition Certification
Nutrition Therapy Institute (NTI) is a leader in holistic nutrition education. Since 1999, NTI has provided students with the highest quality in nutrition training by offering comprehensive holistic nutrition courses online and in-person to help students achieve thriving careers as holistic nutrition therapists in the field of holistic nutrition counseling and wellness. Interested in starting our holistic nutrition courses and earning your holistic nutrition certification? Attend an informational webinar to learn more by signing up HERE.
Images: Image by Clker-Free-Vector-Images is free for use by Pixabay; Image by Jatlas is licensed under CC BY-SA 3.0; Image by divotomezove is free for use by Pixabay; Image by cattalin is free for use by Pixabay
Share this post!




















